Top of the pageCheck Your Symptoms
Overview
The cause of abdominal problems, or belly problems, can be hard to find. Sometimes minor and serious belly problems start with the same symptoms. Most of these problems are minor. In these cases, home treatment is all that's needed.
How severe your pain is, its location, and other symptoms you have may help find what is causing the pain.
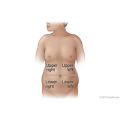
- Generalized pain occurs in half of the belly or more. This pain can occur with many different illnesses. Most often it will go away without medical treatment. Indigestion and a stomach infection are common problems that can cause this type of pain. Home treatment may help relieve some of the discomfort. Generalized mild pain or crampy pain that gets worse over several hours may be a symptom that the intestines are blocked (bowel obstruction).
- Localized pain is in one area of the belly. Localized pain that starts all of a sudden and gets worse is more likely to be a symptom of a serious problem. The pain of appendicitis may start as generalized pain, but it often moves (localizes) to one area of the belly. The pain from gallbladder disease or peptic ulcer disease often starts in one area of the belly and stays in that same place. Localized pain that slowly gets worse may be a symptom of inflammation of an organ in the belly.
- Cramping is a type of pain that comes and goes (intermittent) or that changes where it is or how bad it is. Cramping is rarely serious if it feels better after you pass gas or a stool. Many people have cramping pain with their menstrual periods. Generalized cramping pain is most often not a problem unless it gets worse, does not go away, or localizes. Cramping that starts all of a sudden with diarrhea or other minor health problems can be quite painful. But it most often isn't serious.
Now and then, severe pain that starts all of a sudden may be a symptom of a rupture of the stomach or intestines (perforation), torsion of the testicle or ovary, a kidney stone, gallbladder disease, or blood vessel problems, such as an aortic aneurysm. The pain caused by appendicitis or gallbladder disease may get worse when you move or cough. Pain that gets worse when you move or cough and that doesn't seem to be caused by strained muscles is more likely to be a symptom of a serious problem. A visit to a doctor is usually needed when severe belly pain starts suddenly, or when new and different mild pain slowly gets worse over several hours or days.
After a minor injury to the belly, you may have pain, nausea, or vomiting that often gets better in a few minutes. Pain and other symptoms that start, keep going, or get worse after an injury may mean that an organ in the belly has been damaged.
Many medicines can cause belly pain. Some also cause side effects, such as constipation, which can make belly pain worse.
Belly symptoms can also occur from an infection passed on by animals or while traveling to a foreign country.
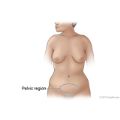
Some belly symptoms have been linked to ovarian cancer. These symptoms include belly or pelvic pain, increased belly size or bloating, trouble eating, and feeling full quickly. If you have one or more of these symptoms, and it occurs almost daily for more than 2 or 3 weeks, talk with your doctor.
Check Your Symptoms
The medical assessment of symptoms is based on the body parts you have.
- If you are transgender or nonbinary, choose the sex that matches the body parts (such as ovaries, testes, prostate, breasts, penis, or vagina) you now have in the area where you are having symptoms.
- If your symptoms aren’t related to those organs, you can choose the gender you identify with.
- If you have some organs of both sexes, you may need to go through this triage tool twice (once as "male" and once as "female"). This will make sure that the tool asks the right questions for you.
Many things can affect how your body responds to a symptom and what kind of care you may need. These include:
- Your age. Babies and older adults tend to get sicker quicker.
- Your overall health. If you have a condition such as diabetes, HIV, cancer, or heart disease, you may need to pay closer attention to certain symptoms and seek care sooner.
- Medicines you take. Certain medicines, such as blood thinners (anticoagulants), medicines that suppress the immune system like steroids or chemotherapy, herbal remedies, or supplements can cause symptoms or make them worse.
- Recent health events, such as surgery or injury. These kinds of events can cause symptoms afterwards or make them more serious.
- Your health habits and lifestyle, such as eating and exercise habits, smoking, alcohol or drug use, sexual history, and travel.
Try Home Treatment
You have answered all the questions. Based on your answers, you may be able to take care of this problem at home.
- Try home treatment to relieve the symptoms.
- Call your doctor if symptoms get worse or you have any concerns (for example, if symptoms are not getting better as you would expect). You may need care sooner.
With cramping pain in the belly:
- The pain may hurt a little or a lot.
- The amount of pain may change from minute to minute. Cramps often get better when you pass gas or have a bowel movement.
- The pain may feel like a tightness or pinching in your belly.
- The pain may be in one specific area or be over a larger area. It may move around.
Shock is a life-threatening condition that may quickly occur after a sudden illness or injury.
Adults and older children often have several symptoms of shock. These include:
- Passing out (losing consciousness).
- Feeling very dizzy or lightheaded, like you may pass out.
- Feeling very weak or having trouble standing.
- Not feeling alert or able to think clearly. You may be confused, restless, fearful, or unable to respond to questions.
If you're not sure if a fever is high, moderate, or mild, think about these issues:
With a high fever:
- You feel very hot.
- It is likely one of the highest fevers you've ever had. High fevers are not that common, especially in adults.
With a moderate fever:
- You feel warm or hot.
- You know you have a fever.
With a mild fever:
- You may feel a little warm.
- You think you might have a fever, but you're not sure.
Temperature varies a little depending on how you measure it. For adults and children age 12 and older, these are the ranges for high, moderate, and mild, according to how you took the temperature.
Oral (by mouth) temperature
- High: 104°F (40°C) and higher
- Moderate: 100.4°F (38°C) to 103.9°F (39.9°C)
- Mild: 100.3°F (37.9°C) and lower
A forehead (temporal) scanner is usually 0.5°F (0.3°C) to 1°F (0.6°C) lower than an oral temperature.
Ear temperature
- High: 105°F (40.6°C) and higher
- Moderate: 101.4°F (38.6°C) to 104.9°F (40.5°C)
- Mild: 101.3°F (38.5°C) and lower
Armpit (axillary) temperature
- High: 103°F (39.5°C) and higher
- Moderate: 99.4°F (37.4°C) to 102.9°F (39.4°C)
- Mild: 99.3°F (37.3°C) and lower
Certain health conditions and medicines weaken the immune system's ability to fight off infection and illness. Some examples in adults are:
- Diseases such as diabetes, cancer, heart disease, and HIV/AIDS.
- Long-term alcohol and drug problems.
- Steroid medicines, which may be used to treat a variety of conditions.
- Chemotherapy and radiation therapy for cancer.
- Other medicines used to treat autoimmune disease.
- Medicines taken after organ transplant.
- Not having a spleen.
Pain in adults and older children
- Severe pain (8 to 10): The pain is so bad that you can't stand it for more than a few hours, can't sleep, and can't do anything else except focus on the pain.
- Moderate pain (5 to 7): The pain is bad enough to disrupt your normal activities and your sleep, but you can tolerate it for hours or days. Moderate can also mean pain that comes and goes even if it's severe when it's there.
- Mild pain (1 to 4): You notice the pain, but it is not bad enough to disrupt your sleep or activities.
It is easy for your diabetes to become out of control when you are sick. Because of an illness:
- Your blood sugar may be too high or too low.
- You may not be able take your diabetes medicine (if you are vomiting or having trouble keeping food or fluids down).
- You may not know how to adjust the timing or dose of your diabetes medicine.
- You may not be eating enough or drinking enough fluids.
An illness plan for people with diabetes usually covers things like:
- How often to test blood sugar and what the target range is.
- Whether and how to adjust the dose and timing of insulin or other diabetes medicines.
- What to do if you have trouble keeping food or fluids down.
- When to call your doctor.
The plan is designed to help keep your diabetes in control even though you are sick. When you have diabetes, even a minor illness can cause problems.
You can get dehydrated when you lose a lot of fluids because of problems like vomiting or fever.
Symptoms of dehydration can range from mild to severe. For example:
- You may feel tired and edgy (mild dehydration), or you may feel weak, not alert, and not able to think clearly (severe dehydration).
- You may pass less urine than usual (mild dehydration), or you may not be passing urine at all (severe dehydration).
Severe dehydration means:
- Your mouth and eyes may be extremely dry.
- You may pass little or no urine for 12 or more hours.
- You may not feel alert or be able to think clearly.
- You may be too weak or dizzy to stand.
- You may pass out.
Moderate dehydration means:
- You may be a lot more thirsty than usual.
- Your mouth and eyes may be drier than usual.
- You may pass little or no urine for 8 or more hours.
- You may feel dizzy when you stand or sit up.
Mild dehydration means:
- You may be more thirsty than usual.
- You may pass less urine than usual.
Blood in the stool can come from anywhere in the digestive tract, such as the stomach or intestines. Depending on where the blood is coming from and how fast it is moving, it may be bright red, reddish brown, or black like tar.
A little bit of bright red blood on the stool or on the toilet paper is often caused by mild irritation of the rectum. For example, this can happen if you have to strain hard to pass a stool or if you have a hemorrhoid.
A large amount of blood in the stool may mean a more serious problem is present. For example, if there is a lot of blood in the stool, not just on the surface, you may need to call your doctor right away. If there are just a few drops on the stool or in the diaper, you may need to let your doctor know today to discuss your symptoms. Black stools may mean you have blood in the digestive tract that may need treatment right away, or may go away on its own.
Certain medicines and foods can affect the color of stool. Diarrhea medicines (such as Pepto-Bismol) and iron tablets can make the stool black. Eating lots of beets may turn the stool red. Eating foods with black or dark blue food coloring can turn the stool black.
If you take aspirin or some other medicine (called a blood thinner) that prevents blood clots, it can cause some blood in your stools. If you take a blood thinner and have ongoing blood in your stools, call your doctor to discuss your symptoms.
Symptoms of a heart attack may include:
- Chest pain or pressure, or a strange feeling in the chest.
- Sweating.
- Shortness of breath.
- Nausea or vomiting.
- Pain, pressure, or a strange feeling in the back, neck, jaw, or upper belly, or in one or both shoulders or arms.
- Lightheadedness or sudden weakness.
- A fast or irregular heartbeat.
For men and women, the most common symptom is chest pain or pressure. But women are somewhat more likely than men to have other symptoms like shortness of breath, tiredness, nausea, and back or jaw pain.
Many prescription and nonprescription medicines can cause belly pain or cramping. A few examples are:
- Aspirin, ibuprofen (such as Advil or Motrin), and naproxen (such as Aleve).
- Antibiotics.
- Antidiarrheals.
- Laxatives.
- Iron supplements.
Call 911 Now
Based on your answers, you need emergency care.
Call 911 or other emergency services now.
Sometimes people don't want to call 911. They may think that their symptoms aren't serious or that they can just get someone else to drive them. Or they might be concerned about the cost. But based on your answers, the safest and quickest way for you to get the care you need is to call 911 for medical transport to the hospital.
Seek Care Now
Based on your answers, you may need care right away. The problem is likely to get worse without medical care.
- Call your doctor now to discuss the symptoms and arrange for care.
- If you cannot reach your doctor or you don't have one, seek care in the next hour.
- You do not need to call an ambulance unless:
- You cannot travel safely either by driving yourself or by having someone else drive you.
- You are in an area where heavy traffic or other problems may slow you down.
Seek Care Today
Based on your answers, you may need care soon. The problem probably will not get better without medical care.
- Call your doctor or telehealth provider today to discuss the symptoms and arrange for care.
- If you cannot reach your doctor or telehealth provider or you don't have one, seek care today.
- If it is evening, watch the symptoms and seek care in the morning.
- If the symptoms get worse, seek care sooner.
What are your options for medical care?
Today your options for where to get your medical care are greater than ever before. You may not even have to leave your home to get the care you want and need. You can choose based on what your health problem is and what works best for you.
- Telehealth is a video call with a health care provider. It can be a convenient way to get medical advice or treatment. Some insurers provide access to telehealth that may be available 24 hours a day. Telehealth for less serious problems may cost less and be faster than in-person clinic visits.
- Urgent care and retail clinics are options if you don't have a doctor, you can't or don't want to wait to see your own doctor, or a telehealth visit can’t treat the problem.
- Virtual care from your primary provider or a telehealth service can be delivered through your smartphone, computer, or tablet.
Make an Appointment
Based on your answers, the problem may not improve without medical care.
- Make an appointment to see your doctor in the next 1 to 2 weeks, or contact your telehealth provider.
- If appropriate, try home treatment while you are waiting for the appointment.
- If symptoms get worse or you have any concerns, call your doctor or telehealth provider. You may need care sooner.
What are your options for medical care?
Today your options for where to get your medical care are greater than ever before. You may not even have to leave your home to get the care you want and need. You can choose based on what your health problem is and what works best for you.
- Telehealth is a video call with a health care provider. It can be a convenient way to get medical advice or treatment. Some insurers provide access to telehealth that may be available 24 hours a day. Telehealth for less serious problems may cost less and be faster than in-person clinic visits.
- Urgent care and retail clinics are options if you don't have a doctor, you can't or don't want to wait to see your own doctor, or a telehealth visit can’t treat the problem.
- Virtual care from your primary provider or a telehealth service can be delivered through your smartphone, computer, or tablet.
Call 911 Now
Based on your answers, you need emergency care.
Call 911 or other emergency services now.
After you call 911, the operator may tell you to chew 1 adult-strength (325 mg) or 2 to 4 low-dose (81 mg) aspirin. Wait for an ambulance. Do not try to drive yourself.
Sometimes people don't want to call 911. They may think that their symptoms aren't serious or that they can just get someone else to drive them. Or they might be concerned about the cost. But based on your answers, the safest and quickest way for you to get the care you need is to call 911 for medical transport to the hospital.
Self-Care
Most of the time, abdominal pain, or belly pain, improves with home treatment, and you don't need to see a doctor. Specific home treatment for mild belly pain often depends on the symptoms you have along with the pain, such as diarrhea or nausea and vomiting.
If you have mild belly pain without other symptoms, the following steps may help you feel better.
- Rest until you feel better.
- Drink plenty of fluids to prevent dehydration.
You may find that taking small, frequent sips of a drink is easier on your stomach than trying to drink a whole glass at once. Don't drink fizzy drinks such as soda pop.
- When you feel like eating, start with small amounts of food.
This will help you get enough nutrition.
- Don't use aspirin or other nonsteroidal anti-inflammatory medicines, such as ibuprofen or naproxen.
These medicines may irritate your stomach and make pain worse.
When to call for help during self-care
Call a doctor if any of the following occur during self-care at home:
- Pain gets worse, does not improve, or is felt in one specific area of the belly.
- Other symptoms develop, such as diarrhea, nausea, vomiting, or a fever.
- The belly feels hard or looks very swollen.
- Symptoms occur more often or are more severe.
Learn more
Preparing For Your Appointment
You can help your doctor diagnose and treat your condition by being prepared for your appointment.
Related Information
Credits
Current as of: October 19, 2024
Author: Ignite Healthwise, LLC Staff
Clinical Review Board
All Ignite Healthwise, LLC education is reviewed by a team that includes physicians, nurses, advanced practitioners, registered dieticians, and other healthcare professionals.
Current as of: October 19, 2024
Author: Ignite Healthwise, LLC Staff
Clinical Review Board
All Ignite Healthwise, LLC education is reviewed by a team that includes physicians, nurses, advanced practitioners, registered dieticians, and other healthcare professionals.