Condition Basics
What is strabismus?
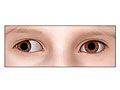
Strabismus (say "struh-BIZ-mus") is a vision problem in which both eyes do not look at the same point at the same time. Strabismus most often begins in early childhood. It is sometimes called crossed-eyes, walleye, or squint.
Normally, the muscles attached to each eye work together to move both eyes in the same direction at the same time. Strabismus occurs when the eye muscles don't work properly to control eye movement. When the eye muscles don't work as they should, the eyes may become misaligned and the brain may not be able to merge what one eye sees with what the other eye sees.
A child rarely outgrows strabismus after it has developed. Without treatment, strabismus can cause permanent vision problems. For example, if the child is not using one eye because it is misaligned, the child can develop poor vision in that eye (called lazy eye or amblyopia).
Having strabismus can be hard on your child's self-esteem. It affects your child's appearance as well as their ability to see well. Other kids may tease your child for being cross-eyed or having a walleye. Be supportive of your child, and seek treatment right away.
What causes it?
Childhood strabismus often has no known cause, although it tends to run in families.
Sometimes strabismus develops when the eyes compensate for other vision problems, such as farsightedness or a cataract. Other things that can increase your child's risk for strabismus include an illness that affects the muscles and nerves, premature birth, Down syndrome, a head injury, and other problems.
Adults may develop strabismus from eye or blood vessel damage. Loss of vision, an eye tumor or a brain tumor, Graves' disease, stroke, and various muscle and nerve disorders can also cause strabismus in adults.
What are the symptoms?
The most common signs of strabismus are:
- Eyes that don't look in the same direction at the same time. (If your child's eyes are only slightly misaligned, you may not notice.)
- Eyes that don't move together.
- Squinting or closing one eye in bright sunlight.
- Tilting or turning the head to look at an object.
- Bumping into things. (Strabismus limits depth perception.)
An older child may also complain about blurred vision, tired eyes, sensitivity to light, or double vision.
Symptoms may come and go. They may get worse when your child is tired or sick.
A newborn's eyes may be misaligned at first. But the eyes should become aligned by 3 to 4 months of age. In some cases, the eyes may simply seem to be misaligned because the child has a wide bridge of the nose that creates the appearance of crossed eyes.
How is it diagnosed?
A doctor can often tell that a child has strabismus just by looking at the child's eyes. It may be obvious that the eyes don't look in the same direction at the same time.
The doctor may have the child look at an object while covering and then uncovering each eye. This allows the doctor to see which eye turns, how much it turns, and under what circumstances the abnormal turn occurs. These tests will also help the doctor find out if the child has amblyopia (lazy eye), which sometimes occurs with strabismus.
Experts recommend that children have regular eye exams. Vision tests may also be done to look for strabismus.footnote 1, footnote 2 If you have concerns about your child's eyes or vision, call your child's doctor, or take your child to an eye doctor.
How is strabismus treated?
Common treatments for strabismus are glasses for mild strabismus or a temporary eye patch to make the weak eye stronger. Other treatments may include medicines and eye exercises. Surgery on the eye muscles can also be done. The earlier you start treatment, the better chances you have of correcting the problem.
Related Information
References
Citations
- U.S. Preventive Services Task Force (2017). Vision screening in children aged 6 months to 5 years: U.S. Preventive Services Task Force recommendation statement. JAMA, 318(9): 836-844. DOI: 10.1001/jama.2017.11260. Accessed August 6, 2018.
- American Academy of Pediatrics, et al. (2016). Policy statement: Visual system assessment in infants, children, and young adults by pediatricians. Pediatrics, 137(1): 28–30. DOI: 10.1542/peds.2015-3596. Accessed March 6, 2017.
Credits
Current as of: October 1, 2025
Author: Ignite Healthwise, LLC Staff
Clinical Review Board
All Ignite Healthwise, LLC education is reviewed by a team that includes physicians, nurses, advanced practitioners, registered dieticians, and other healthcare professionals.
Current as of: October 1, 2025
Author: Ignite Healthwise, LLC Staff
Clinical Review Board
All Ignite Healthwise, LLC education is reviewed by a team that includes physicians, nurses, advanced practitioners, registered dieticians, and other healthcare professionals.