Condition Basics
What is supraventricular tachycardia (SVT)?
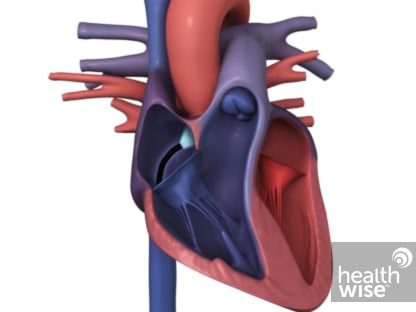
Supraventricular tachycardia (SVT) means that from time to time your heart beats very fast for a reason other than exercise, high fever, or stress. For most people who have SVT, the heart still works normally to pump blood through the body.
During an episode of SVT, the heart's electrical system doesn't work right, causing the heart to beat very fast. The heart beats at least 100 beats a minute and may reach 250 beats a minute or more. After treatment or on its own, the heart usually returns to a normal rate of about 60 to 100 beats a minute.
SVT may start and end quickly, and you may not have symptoms. SVT becomes a problem when it happens often, lasts a long time, or causes symptoms.
What causes it?
Most episodes of SVT are caused by faulty electrical connections in the heart. Some types of SVT may run in families, such as Wolff-Parkinson-White syndrome. SVT also can be caused by certain health problems, heart and lung medicines, or surgery.
What are the symptoms?
When your heart is beating fast from SVT, you may feel a fluttering in your chest (palpitations) and have a fast pulse. You may feel lightheaded, be short of breath, or feel discomfort in the chest. Some people with SVT have no symptoms.
How is it diagnosed?
Your doctor may diagnose SVT based on a physical exam, your symptoms and history, and a test called an electrocardiogram (EKG, ECG). You may need other tests such as an electrophysiology study, blood tests, chest X-rays, or an echocardiogram to identify what type of SVT you have or find the cause.
How is SVT treated?
SVT does not always need to be treated. If needed, treatment options include medicine, cardioversion, and a procedure called catheter ablation. Your doctor may also teach you how to slow your heart rate on your own with physical actions called vagal maneuvers. You and your doctor can decide what treatment is right for you.
Symptoms
Symptoms of SVT include:
- A racing or fluttering feeling in the chest (palpitations).
- Chest discomfort, such as pressure, tightness, or pain.
- Fainting, or feeling lightheaded or dizzy.
- Shortness of breath.
- A pounding pulse. You may feel or see your pulse beating, especially at your neck, where large blood vessels are close to the skin.
- Sweating.
Some people with SVT have no symptoms.
When to Call a Doctor
Call 911 or seek emergency services immediately if you have a fast heart rate and you:
- Faint or feel as though you are going to faint.
- Have severe shortness of breath.
- Have chest pain.
- Have symptoms of a heart attack or stroke.
Call your doctor if you feel fluttering in your chest (palpitations) that persists and doesn't go away quickly or if you have frequent palpitations.
Exams and Tests
Your doctor will diagnose SVT based on your health and symptoms, a physical exam, and your test results. Your doctor:
- Will ask if anything triggers the fast heart rate, how long it lasts, if it starts and stops suddenly, and if the beats are regular or irregular.
- Will do a test called an electrocardiogram (EKG, ECG). This test measures the heart's electrical activity and can record SVT episodes.
If you do not have an episode of SVT while you're at the doctor's office, your doctor probably will ask you to wear a portable electrocardiogram (EKG), also called an ambulatory electrocardiogram. When you have an episode, the device will record it.
Your doctor also may do tests to find the cause of the SVT. These may include blood tests, a chest X-ray, and an echocardiogram, which shows the heart in motion.
Learn more
Treatment Overview
Some SVTs don't cause symptoms, and you may not need treatment. If you do have symptoms, your doctor probably will recommend treatment.
To treat sudden episodes of SVT, your doctor may:
- Prescribe a medicine to take when the SVT occurs.
- Show you how you can slow your heart rate on your own with physical actions. These actions are called vagal maneuvers. They include bearing down or putting an ice-cold, wet towel on your face.
If these treatments don't work, you may have to go to your doctor's office or the emergency room. You may get a fast-acting medicine to slow your heart rate. If the SVT is serious, you may have a procedure called electrical cardioversion to reset the heart rhythm.
The goals of treatment are to prevent episodes, relieve symptoms, and prevent future problems. You and your doctor can decide what type of treatment is right for you. Your options may include medicines or a procedure called catheter ablation.
Catheter ablation might be done if you have symptoms that bother you a lot, you don't want to take heart rhythm medicine, or medicine has not worked for you. Ablation has risks, but they are rare. Many people decide to have ablation because they hope to feel much better afterward. That hope is worth the risks to them. But the risks may not be worth it for people who have few symptoms. Work with your doctor to decide what treatment is right for you.
Learn more
Watch
Self-Care
When you have SVT, you can monitor your heart rate and learn ways to slow it down when you have symptoms.
- Keep a diary of your heart rate and symptoms.
This helps you monitor your episodes and symptoms. Bring this diary to your doctor appointments. It may also help you identify things—such as drinking alcohol or smoking—that trigger episodes.
- Check your pulse when you have symptoms, and record the information in your diary.
Be aware that if your heart is beating rapidly, it may be hard to feel your pulse and get an accurate count of your actual heart rate.
- Try vagal maneuvers—such as holding your breath and bearing down or putting an ice-cold, wet towel on your face—to slow your heart rate.
Your doctor will help you learn these procedures so you can try them at home when your fast heart rate occurs.
- If you smoke, try to quit or cut back as much as you can.
If you need help quitting, talk to your doctor about stop-smoking programs and medicines. These can increase your chances of quitting for good.
- Avoid or limit alcohol if it causes symptoms.
- Avoid medicines and supplements that contain stimulants.
This includes decongestants like oxymetazoline (such as Afrin and other brands) and pseudoephedrine (such as Sudafed and other brands). Doctors also warn against using diet pills or "pep" pills, ephedrine, ephedra, the herb ma huang, or other stimulants.
- Avoid or limit caffeine if it causes symptoms.
For most people, moderate amounts of caffeine do not trigger SVT. So most people do not have to avoid chocolate, caffeinated coffee, tea, or soft drinks.
- If you use stimulant drugs, quit or cut back as much as you can.
These drugs include cocaine and methamphetamine. It's safest not to use them at all. Talk to your doctor if you need help decreasing your use.
Learn more
Watch
Related Information
Credits
Current as of: July 31, 2024
Author: Ignite Healthwise, LLC Staff
Clinical Review Board
All Healthwise education is reviewed by a team that includes physicians, nurses, advanced practitioners, registered dieticians, and other healthcare professionals.
Current as of: July 31, 2024
Author: Ignite Healthwise, LLC Staff
Clinical Review Board
All Healthwise education is reviewed by a team that includes physicians, nurses, advanced practitioners, registered dieticians, and other healthcare professionals.