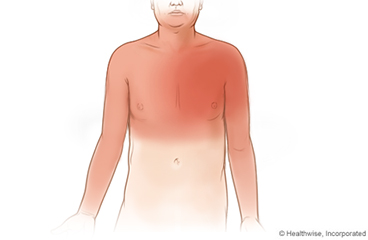
What is stable angina?
Angina is a symptom of coronary artery disease. For most people, it feels like chest pain or pressure. Some people feel other symptoms. These symptoms include pain, pressure, or a strange feeling in the back, neck, jaw, or upper belly, or in one or both shoulders or arms.
The most common types of angina are stable angina and unstable angina. Stable angina means that you can usually predict when your symptoms will happen. You probably know what things cause your angina. (With unstable angina, your symptoms have changed. They don't follow your typical pattern of stable angina.)
Most people who have stable angina can manage their symptoms. This includes taking medicines as prescribed and knowing when to call the doctor or get help right away. It also includes paying attention to your symptoms so you can see what causes them and what is typical for you.
What can you do to manage angina?
Be aware of your symptoms
Tracking when and why your angina symptoms happen is one way to understand your angina better. It also helps you know what's normal for you.
If you know what's normal for you, it'll be easier to tell if you have a change in symptoms that means it's time to call for help.
Understanding your normal patterns may also help you make some changes that might prevent or reduce symptoms.
To track your symptoms, write down:
- The day and time of day you notice symptoms.
- What you were doing when you had them:
- Exercising or doing a physical activity?
- Eating a large meal?
- Spending time outside in very cold weather?
- Feeling a lot of stress?
- Something else?
- How long the symptoms lasted.
- What you did to help your symptoms.
Work with your doctor
You and your doctor can use your symptoms tracking information to talk about whether you need any changes to your angina treatment. For example, you may decide to use medicine or to change your medicine. Or you may talk about other treatments you could try. Most people who have stable angina can control their symptoms by taking prescribed medicines, including nitroglycerin, when needed.
Balance activity and rest
Staying active and knowing when to rest during activity are also important.
Here are some tips that might help you manage your angina.
- Ease into your day.
- Warm up slowly before activity. Talk to your doctor about a level of activity that is safe for you.
- Give yourself time to rest and digest right after meals.
- Change the way you eat. Eat smaller meals more often during the day instead of two or three large meals.
- If an activity causes angina, stop and rest. Be active at a level that does not cause symptoms.
When should you call for help?
Call 911 anytime you think you may need emergency care. For example, call if:
- You passed out (lost consciousness).
- You have symptoms of a heart attack. These may include:
- Chest pain or pressure, or a strange feeling in the chest.
- Sweating.
- Shortness of breath.
- Nausea or vomiting.
- Pain, pressure, or a strange feeling in the back, neck, jaw, or upper belly or in one or both shoulders or arms.
- Lightheadedness or sudden weakness.
- A fast or irregular heartbeat.
- You have angina symptoms that do not go away with rest or are not getting better within 5 minutes after you take a dose of nitroglycerin.
Call your doctor now if:
- Your angina symptoms seem worse but still follow your typical pattern. You can predict when symptoms will happen, but they may come on sooner, feel worse, or last longer.
- You feel dizzy or lightheaded, or you feel like you may faint.
Watch closely for changes in your health, and be sure to contact your doctor if you have any problems.
Follow-up care is a key part of your treatment and safety. Be sure to make and go to all appointments, and call your doctor if you are having problems. It's also a good idea to know your test results and keep a list of the medicines you take.
Where can you learn more?
Go to http://www.healthwise.net/patientEd
Enter V574 in the search box to learn more about "Learning About Managing Stable Angina".
Current as of: October 2, 2025
Author: Ignite Healthwise, LLC Staff
Clinical Review Board
All Ignite Healthwise, LLC education is reviewed by a team that includes physicians, nurses, advanced practitioners, registered dieticians, and other healthcare professionals.

