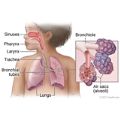
What is respiratory syncytial virus (RSV) infection?
Respiratory syncytial virus infection (RSV) is a lot like a bad cold. It causes the same symptoms. And like a cold, it's very common and spreads easily. Most children have it at least once by age 2. It may take older adults longer to recover from RSV and any problems caused by the infection.
What causes it?
A virus causes RSV infection. Like a cold virus, RSV attacks your nose, eyes, throat, and lungs. There are two main types of RSV and many subtypes (strains), so your body never becomes immune to it. You can get it again and again throughout your life. Sometimes during the same season.
What are the symptoms?
RSV usually causes the same symptoms as a bad cold, such as a cough, a stuffy or runny nose, a mild sore throat, an earache, and a fever. Babies with RSV may also have low energy, act fussy or cranky, or be less hungry than usual. Some children have more serious symptoms, like wheezing.
How is it diagnosed?
Doctors usually diagnose RSV by asking about the symptoms. There are tests for RSV, but they usually aren't needed. Your doctor may want to do testing if you or your child may be likely to have other problems. The most common test collects a sample of the fluid in the back of the nose.
How is RSV treated?
RSV usually goes away on its own. Home treatment is often all that's needed. You can help relieve symptoms by giving medicine to stop a fever and by drinking enough fluids.
How It Spreads
RSV is very contagious. This means that it spreads easily from person to person.
People with RSV infection may spread the virus through their secretions (saliva or mucus) when they cough, sneeze, talk, or share food or drink. You can catch the virus by:
- Touching an object or surface that has the virus on it and then touching your nose, eyes, or mouth without first washing your hands. The virus can survive for many hours on countertops and other hard surfaces, such as doorknobs. It can survive for a shorter time on hands, clothing, or tissue.
- Close contact. If an infected person coughs or sneezes near you, you could breathe in RSV that's in that person's saliva or mucus.
The virus spreads easily in crowded settings, such as child care centers, preschools, and nursing homes. Children who go to school often spread the virus to their parents and siblings.
Prevention
It's very hard to keep from catching RSV, just like it's hard to keep from catching a cold. But you can lower the chances by practicing good health habits. Wash your hands often, and teach children to do the same.
To prevent RSV in older adults, an RSV vaccine is recommended for anyone age 75 or older. It is also recommended for adults ages 50 to 74 who are at increased risk for severe RSV.
There are two immunization options recommended to protect all babies from severe RSV. Only one of these options is usually needed for most babies to be protected:
- The RSV vaccine given during 32 to 36 weeks of pregnancy and right before or during RSV season. Immunity is then passed to the baby during pregnancy.
- RSV antibodies given to babies who are younger than 8 months and born during or at the start of RSV season. RSV antibodies may also be advised for some babies and young children ages 8 months through 19 months who are at increased risk for severe RSV.
Symptoms
RSV usually causes the same symptoms as a bad cold, such as:
- A cough.
- A stuffy or runny nose.
- A mild sore throat.
- An earache.
- A fever, usually at the start of the illness. A high fever doesn't mean the illness is more severe.
Babies with RSV may also:
- Have a decreased interest in their surroundings.
- Have low energy. They may be listless and sleepy.
- Act fussy or cranky.
- Not sleep well.
- Be less hungry than usual.
- Have apnea, where breathing stops for about 15 to 20 seconds. This usually occurs only in babies who were born prematurely and who also have a history of apnea.
Some children have other serious symptoms, like wheezing. Call your doctor if your child is wheezing or having trouble breathing.
RSV infection sometimes leads to bronchiolitis, pneumonia, or both.
What Happens
RSV spreads easily and is very hard to avoid.
Children who have only upper respiratory system symptoms, such as a sore throat or a runny nose, usually recover in about 10 to 14 days. A child's first RSV infection, which almost always occurs by age 2, usually is the most severe. Some babies and children have a higher risk of other problems caused by RSV because of a health condition or another problem. There are medicines available for babies and young children that can help prevent infection. You can talk with your child's doctor about getting those medicines. In young children, the most common problems caused by RSV are bronchiolitis and pneumonia.
Older adults have a higher risk of problems caused by RSV. It may take older adults longer to recover from RSV and any problems caused by it. Adults ages 50 to 74 who are at increased risk can get a vaccine to prevent infection. The vaccine is recommended for all adults ages 75 and older. The risk of problems from getting RSV is even higher if there are other health problems, such as pneumonia, chronic obstructive pulmonary disease (COPD), or heart failure.
You may be able to get an RSV vaccine during pregnancy, which can then help prevent your infant from getting the infection. Talk to your doctor about your options.
When to Call a Doctor
Call 911 or other emergency services immediately if:
- Your child has severe trouble breathing.
- Your child's breathing has stopped.
- Start rescue breathing.
Call your doctor now if your baby or child has moderate trouble breathing .
Call a doctor if your child:
- Breathes slightly faster than normal and seems to be getting worse. Most healthy children breathe less than 40 times a minute.
- Has cold symptoms that become severe.
- Has shallow coughing, which continues throughout the day and night.
- Has a poor appetite or is being less active than usual.
- Has any trouble breathing.
Watchful waiting
Watch your child closely if there are symptoms of an upper respiratory infection. There are medicines available for babies and young children that can help prevent infection. You can talk with your child's doctor about getting those medicines.
Exams and Tests
Doctors usually diagnose RSV by asking about your or your child's symptoms and by knowing if there's an outbreak of the infection in your area.
There are tests for RSV, but they usually aren't needed. Your doctor may want to do testing if you or your child may be likely to have other problems. A viral detection test may be done to confirm a diagnosis of RSV in children and older adults who have symptoms and who are at high risk for a severe infection or for complications.
The test uses a sample of the drainage from the nose, obtained with a cotton swab or nasal wash. Testing may also be recommended for people who are in the hospital if the cause of symptoms hasn't already been found and they have a high risk of having complications.
The results of viral detection tests help doctors know if precautions are needed to prevent the spread of infection. For children who are at risk for getting severe infections or complications of RSV infections, the results of these tests may help guide treatment, such as the need for medicines.
Certain tests may be needed if RSV symptoms don't improve or if they get worse. Or they may be needed if complications such as bronchiolitis or pneumonia are suspected. These tests may include:
- A chest X-ray. This test may show signs of pneumonia.
- Blood tests. These may include a chemistry screening, a complete blood count, or arterial blood gases analysis.
- Oximetry. This test measures the amount of oxygen in the blood.
Treatment Overview
RSV usually goes away on its own. Home treatment is often all that's needed. When someone with RSV is otherwise healthy, symptoms usually get better in a week or two.
If your child has RSV:
- Use saline drops to thin mucus. Suction your baby's nose if your baby can't breathe well enough to eat or sleep.
- Give your child acetaminophen (Tylenol) or ibuprofen (Advil, Motrin) for fever. Do not use ibuprofen if your child is less than 6 months old unless the doctor gave you instructions to use it. Be safe with medicines. Read and follow all instructions on the label. Do not give aspirin to children and teens. It has been linked to Reye syndrome, a rare but serious illness.
RSV can be serious when the symptoms are very bad or when it leads to other problems. Certain people, like babies and people with immune system problems, are more likely to have problems with RSV. These people sometimes need treatment in a hospital.
Self-Care
Take medicines exactly as prescribed. Drink lots of fluids. Take acetaminophen (Tylenol) or ibuprofen (Advil, Motrin) to help with a fever if your doctor says it's okay. Use an extra pillow to prop up your head to make it easier to sleep.
Caring for your child
- Be safe with medicines. Have your child take medicine exactly as prescribed. Do not stop or change a medicine without talking to your child's doctor first.
- Give your child lots of fluids. Offer your baby breastfeeding or bottle-feeding more often. Do not give your baby sports drinks, soft drinks, or undiluted fruit juice, as these may have too much sugar, too few calories, or not enough minerals.
- Give your child sips of water or drinks such as Pedialyte or Infalyte. These drinks contain the right mix of salt, sugar, and minerals. You can buy them at drugstores or grocery stores. Do not use them as the only source of liquids or food for more than 12 to 24 hours.
- If your child has problems breathing because of a stuffy nose, squirt a few saline (saltwater) nasal drops in one nostril. For older children, have them blow their nose. Repeat for the other nostril. For babies, put a drop or two in one nostril. Using a soft rubber suction bulb, squeeze air out of the bulb, and gently place the tip of the bulb inside the baby's nose. Relax your hand to suck the mucus from the nose. Repeat in the other nostril.
- Give acetaminophen (Tylenol) or ibuprofen (Advil, Motrin) for fever, pain, or fussiness. Do not use ibuprofen if your child is less than 6 months old unless the doctor gave you instructions to use it. Be safe with medicines. Read and follow all instructions on the label.
- Do not give aspirin to children and teens. It has been linked to Reye syndrome, a rare but serious illness.
- Be careful with cough and cold medicines. Don't give them to children younger than 6, because they don't work for children that age and can even be harmful. For children 6 and older, always follow all the instructions carefully. Make sure you know how much medicine to give and how long to use it. And use the dosing device if one is included.
- Be careful when giving your child over-the-counter cold or flu medicines and Tylenol at the same time. Many of these medicines have acetaminophen, which is Tylenol. Read the labels to make sure that you are not giving your child more than the recommended dose. Too much acetaminophen (Tylenol) can be harmful.
- Keep your child away from smoke. Smoke irritates the breathing tubes and slows healing.
- Let your child rest. Unless you see signs of dehydration, don't wake up your child during naps or at night to take fluids.
Related Information
Credits
Current as of: October 6, 2025
Author: Ignite Healthwise, LLC Staff
Clinical Review Board
All Ignite Healthwise, LLC education is reviewed by a team that includes physicians, nurses, advanced practitioners, registered dieticians, and other healthcare professionals.
Current as of: October 6, 2025
Author: Ignite Healthwise, LLC Staff
Clinical Review Board
All Ignite Healthwise, LLC education is reviewed by a team that includes physicians, nurses, advanced practitioners, registered dieticians, and other healthcare professionals.