Top of the pageCheck Your Symptoms
Overview
Minor arm problems, such as sore muscles, are common. Symptoms often are caused by everyday wear and tear or overuse. Arm problems may be minor or serious. They may include symptoms such as pain, swelling, cramps, numbness, tingling, weakness, or changes in temperature or color.
Older adults have a greater chance of having arm problems. That's because they lose muscle mass as they age. Children may have arm problems because they are usually more active than adults. And children's bones and muscles are growing more quickly. They may also have arm problems for the same reasons as adults.
Your arm problem may be caused by sports or hobbies, work-related tasks, or work or projects around the home. Arm problems can also be caused by injuries.
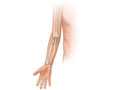
It may be helpful to know the structure of the arm to better understand arm problems. Common arm problems that aren't caused by a specific injury, such as a blow or fall, include:
- Overuse or repetitive-motion injuries. They can occur when you "overdo" an activity or repeat the same activity. The repeated activity may stress joints or other tissues and cause pain and swelling. This is called an overuse injury, even though no obvious injury occurred. For example, you may have shoulder pain from throwing a ball or raking leaves. Overuse injuries include bursitis and tendinitis. Carpal tunnel syndrome is another example.
- Joint pain, stiffness, and swelling. They are common with arthritis. Osteoarthritis (also called degenerative joint disease) is the most common type of arthritis. Less common types include rheumatoid arthritis and lupus.
- Swelling of the hands and arms. It can be caused by hormone changes, such as those that occur during pregnancy or with premenstrual syndrome (PMS).
- Swelling that occurs after surgery to remove the lymph nodes under the arm following a diagnosis of breast cancer or melanoma. This is called lymphedema.
- Arm problems that occur as symptoms of other more serious problems, such as a heart attack, a transient ischemic attack (TIA), or a stroke. Sometimes the first symptom of a heart attack is pain in the left arm.
Most minor arm problems will usually get better on their own. Home treatment may be all that's needed.
Health Tools
Health Tools help you make wise health decisions or take action to improve your health.
Check Your Symptoms
The medical assessment of symptoms is based on the body parts you have.
- If you are transgender or nonbinary, choose the sex that matches the body parts (such as ovaries, testes, prostate, breasts, penis, or vagina) you now have in the area where you are having symptoms.
- If your symptoms aren’t related to those organs, you can choose the gender you identify with.
- If you have some organs of both sexes, you may need to go through this triage tool twice (once as "male" and once as "female"). This will make sure that the tool asks the right questions for you.
Many things can affect how your body responds to a symptom and what kind of care you may need. These include:
- Your age. Babies and older adults tend to get sicker quicker.
- Your overall health. If you have a condition such as diabetes, HIV, cancer, or heart disease, you may need to pay closer attention to certain symptoms and seek care sooner.
- Medicines you take. Certain medicines, such as blood thinners (anticoagulants), medicines that suppress the immune system like steroids or chemotherapy, herbal remedies, or supplements can cause symptoms or make them worse.
- Recent health events, such as surgery or injury. These kinds of events can cause symptoms afterwards or make them more serious.
- Your health habits and lifestyle, such as eating and exercise habits, smoking, alcohol or drug use, sexual history, and travel.
Try Home Treatment
You have answered all the questions. Based on your answers, you may be able to take care of this problem at home.
- Try home treatment to relieve the symptoms.
- Call your doctor if symptoms get worse or you have any concerns (for example, if symptoms are not getting better as you would expect). You may need care sooner.
Symptoms of infection may include:
- Increased pain, swelling, warmth, or redness in or around the area.
- Red streaks leading from the area.
- Pus draining from the area.
- A fever.
Certain health conditions and medicines weaken the immune system's ability to fight off infection and illness. Some examples in adults are:
- Diseases such as diabetes, cancer, heart disease, and HIV/AIDS.
- Long-term alcohol and drug problems.
- Steroid medicines, which may be used to treat a variety of conditions.
- Chemotherapy and radiation therapy for cancer.
- Other medicines used to treat autoimmune disease.
- Medicines taken after organ transplant.
- Not having a spleen.
Pain in children under 3 years
It can be hard to tell how much pain a baby or toddler is in.
- Severe pain (8 to 10): The pain is so bad that the baby cannot sleep, cannot get comfortable, and cries constantly no matter what you do. The baby may kick, make fists, or grimace.
- Moderate pain (5 to 7): The baby is very fussy, clings to you a lot, and may have trouble sleeping but responds when you try to comfort him or her.
- Mild pain (1 to 4): The baby is a little fussy and clings to you a little but responds when you try to comfort him or her.
Pain in children 3 years and older
- Severe pain (8 to 10): The pain is so bad that the child can't stand it for more than a few hours, can't sleep, and can't do anything else except focus on the pain. No one can tolerate severe pain for more than a few hours.
- Moderate pain (5 to 7): The pain is bad enough to disrupt the child's normal activities and sleep, but the child can tolerate it for hours or days.
- Mild pain (1 to 4): The child notices and may complain of the pain, but it is not bad enough to disrupt his or her sleep or activities.
Pain in adults and older children
- Severe pain (8 to 10): The pain is so bad that you can't stand it for more than a few hours, can't sleep, and can't do anything else except focus on the pain.
- Moderate pain (5 to 7): The pain is bad enough to disrupt your normal activities and your sleep, but you can tolerate it for hours or days. Moderate can also mean pain that comes and goes even if it's severe when it's there.
- Mild pain (1 to 4): You notice the pain, but it is not bad enough to disrupt your sleep or activities.
Symptoms of a heart attack may include:
- Chest pain or pressure, or a strange feeling in the chest.
- Sweating.
- Shortness of breath.
- Nausea or vomiting.
- Pain, pressure, or a strange feeling in the back, neck, jaw, or upper belly, or in one or both shoulders or arms.
- Lightheadedness or sudden weakness.
- A fast or irregular heartbeat.
For men and women, the most common symptom is chest pain or pressure. But women are somewhat more likely than men to have other symptoms like shortness of breath, tiredness, nausea, and back or jaw pain.
When an area turns blue, very pale, or cold, it can mean that there has been a sudden change in the blood supply to the area. This can be serious.
There are other reasons for color and temperature changes. Bruises often look blue. A limb may turn blue or pale if you leave it in one position for too long, but its normal color returns after you move it. What you are looking for is a change in how the area looks (it turns blue or pale) and feels (it becomes cold to the touch), and this change does not go away.
Seek Care Now
Based on your answers, you may need care right away. The problem is likely to get worse without medical care.
- Call your doctor now to discuss the symptoms and arrange for care.
- If you cannot reach your doctor or you don't have one, seek care in the next hour.
- You do not need to call an ambulance unless:
- You cannot travel safely either by driving yourself or by having someone else drive you.
- You are in an area where heavy traffic or other problems may slow you down.
Call 911 Now
Based on your answers, you need emergency care.
Call 911 or other emergency services now.
After you call 911, the operator may tell you to chew 1 adult-strength (325 mg) or 2 to 4 low-dose (81 mg) aspirin. Wait for an ambulance. Do not try to drive yourself.
Sometimes people don't want to call 911. They may think that their symptoms aren't serious or that they can just get someone else to drive them. Or they might be concerned about the cost. But based on your answers, the safest and quickest way for you to get the care you need is to call 911 for medical transport to the hospital.
Seek Care Today
Based on your answers, you may need care soon. The problem probably will not get better without medical care.
- Call your doctor today to discuss the symptoms and arrange for care.
- If you cannot reach your doctor or you don't have one, seek care today.
- If it is evening, watch the symptoms and seek care in the morning.
- If the symptoms get worse, seek care sooner.
Call 911 Now
Based on your answers, you need emergency care.
Call 911 or other emergency services now.
Sometimes people don't want to call 911. They may think that their symptoms aren't serious or that they can just get someone else to drive them. Or they might be concerned about the cost. But based on your answers, the safest and quickest way for you to get the care you need is to call 911 for medical transport to the hospital.
Make an Appointment
Based on your answers, the problem may not improve without medical care.
- Make an appointment to see your doctor in the next 1 to 2 weeks.
- If appropriate, try home treatment while you are waiting for the appointment.
- If symptoms get worse or you have any concerns, call your doctor. You may need care sooner.
Self-Care
Try the following tips to help relieve arm pain, swelling, and stiffness.
- Remove jewelry.
Remove rings, bracelets, watches, and any other jewelry from your hand and arm. It will be hard to remove the jewelry after swelling starts.
- Rest.
It's important to rest and protect the affected area. Stop, change, or take a break from any activity that may be causing your pain or soreness.
- Use ice.
Put ice or a cold pack on your arm for 10 to 20 minutes at a time. Try to do this every 1 to 2 hours for the next 3 days (when you are awake).
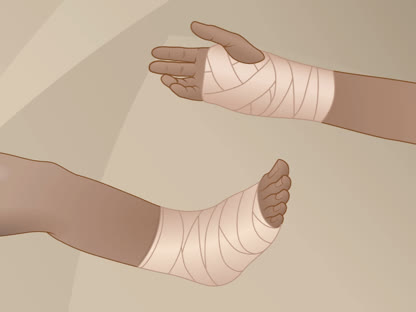
- Wrap the affected area.
Compression, or wrapping the area with an elastic bandage (such as an Ace wrap), will help reduce swelling.
- Don't wrap it too tightly, because that can cause more swelling below the affected area. Loosen the bandage if it gets too tight. Signs that the bandage is too tight include numbness, tingling, increased pain, coolness, and swelling in the area below the bandage.
- Elevate the affected area.
Try to keep the area at or above the level of your heart to help reduce swelling. Prop up the area on pillows while you apply ice and anytime you sit or lie down.
- Wear a sling.
If it makes you more comfortable and supports the affected area, wear a sling.
- Avoid things that might increase swelling.
For 48 hours, avoid things that might increase swelling. These things include hot showers, hot tubs, hot packs, and drinks that contain alcohol.
- Apply heat.
- After 2 or 3 days, you can try applying heat to the area that hurts. Types of heat therapy include microwavable packs and disposable heating patches.
- Apply heat for 10 to 20 minutes at a time.
- You might also try switching between cold and heat.
- Rub the area.
Gently massage or rub the area to relieve pain and encourage blood flow. Don't massage the affected area if it causes pain.
- Don't smoke or use other tobacco products.
Smoking slows healing because it decreases blood supply and delays tissue repair.
If you need to use a wrap or a sling for more than 48 hours, you may have a more serious injury that needs to be checked by a doctor.
Relieving muscle cramps in your arm
Try the following tips to help relieve arm cramps.
- Gently stretch the cramping muscle.
- Rub the area.
If you don't have swelling, you may rub or gently massage the cramp.
- Stay hydrated.
If you think that your muscle cramps are brought on by exercise, heat, or dehydration, drink some extra water. Avoid drinks that contain caffeine or alcohol.
- Move your arms, and flex your fingers and hands.
Gentle motion may help with cramps brought on by exercise.
- Make sure that you are getting enough minerals such as calcium and magnesium.
Most people get enough minerals by eating a normal variety of foods. Talk with your doctor about taking extra calcium.
When to call for help during self-care
Call a doctor if any of the following occur during self-care at home:
- New or worse pain or swelling.
- New signs of infection, such as redness, warmth, pus, or a fever.
- New or worse numbness, tingling, or cool and pale skin.
- Movement or strength decreases.
- Symptoms occur more often or are more severe.
Learn more
Watch
Preparing For Your Appointment
You can help your doctor diagnose and treat your condition by being prepared for your appointment.
Related Information
Credits
Current as of: July 31, 2024
Author: Ignite Healthwise, LLC Staff
Clinical Review Board
All Healthwise education is reviewed by a team that includes physicians, nurses, advanced practitioners, registered dieticians, and other healthcare professionals.
Current as of: July 31, 2024
Author: Ignite Healthwise, LLC Staff
Clinical Review Board
All Healthwise education is reviewed by a team that includes physicians, nurses, advanced practitioners, registered dieticians, and other healthcare professionals.