What is it?
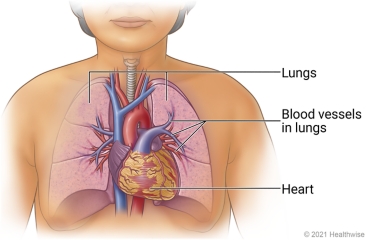
A lung scan is a type of nuclear scanning test. It uses a special camera to take pictures of the lungs after a radioactive tracer is put into the body. It is most often used to find a pulmonary embolism. This is a blood clot that prevents normal blood flow in the lung.
Two types of lung scans are usually done together. They are:
- Ventilation scan.
- You inhale a radioactive tracer gas or mist. Pictures from this scan can show areas of the lungs that aren't getting enough air or that hold too much air.
- Perfusion scan.
- A radioactive tracer is injected into a vein in your arm. It travels through your blood and into the lungs. Pictures from this scan can show areas of the lungs that aren't getting enough blood.
If both scans are done, the test is called a V/Q scan. The ventilation scan usually is done first.
In most cases, if the lungs are working as they should, both scans will show that the parts of the lungs that are getting air are also getting blood. If the two scan results don't match, the differences can help your doctor diagnose a problem with your lungs.
Lung scan results can help your doctor find out how likely it is that you have a blood clot in your lung. If there is a chance that you have a blood clot, your doctor may order more tests. If the chance is high, your doctor may give you medicine to treat the clot.
Why is this test done?
A lung scan is done to:
- Find a blood clot that is preventing normal blood flow to part of a lung.
- Look at the flow of blood or air through the lungs.
- See which parts of the lungs are working and which are damaged. This is often done before surgery to remove parts of the lung.
How do you prepare for the test?
If you are breastfeeding, you may want to pump enough breast milk before the test to get through 1 to 2 days of feeding. The radioactive tracer used in this test can get into your breast milk and is not good for the baby.
How is the test done?
During the scans, the camera may move to take pictures from different angles.
Ventilation scan
- A mask will be placed over your mouth and nose. Or you may have a nose clip on your nose and a tube in your mouth that you use for breathing. You will take a deep breath and hold it.
- The camera will take pictures as the tracer moves into your lungs.
- You may be asked to breathe the gas in and out through your mouth for several minutes and then to hold your breath for short periods (about 10 seconds). You may have to change positions so your lungs can be viewed from other angles.
- Afterward, the gas or mist will clear from your lungs as you breathe.
Perfusion scan
- A small amount of the tracer will be injected into your arm.
- The camera will take pictures as the tracer moves through the blood vessels in your lungs.
How long does the test take?
The two scans are usually done together and will take about an hour. The ventilation scan takes about 15 to 30 minutes, and the perfusion scan takes about 5 to 10 minutes. The scans can be done on their own.
What are the risks of this test?
- Allergic reactions to the radioactive tracer are very rare.
- Anytime you're exposed to radiation, there's a small chance of damage to cells or tissue. That's the case even with the low-level radioactive tracer used for this test. But the chance of damage is very low compared with the benefits of the test.
What happens after the test?
- Most of the tracer will leave your body through your urine or stool within a day. So be sure to flush the toilet right after you use it, and wash your hands well with soap and water. The amount of radiation in the tracer is very small. This means it isn't a risk for people to be around you after the test.
- After the test, drink lots of fluids for the next 24 hours to help flush the tracer out of your body.
- Radioactive tracer used in this test can get into your breast milk. Do not breastfeed your baby for 1 or 2 days after this test. During this time, you can give your baby breast milk you stored before the test, or you can give formula. Discard the breast milk you pump in the 1 or 2 days after the test.
- Some people have soreness or swelling at the injection site. A moist, warm compress applied to the arm may help.
Follow-up care is a key part of your treatment and safety. Be sure to make and go to all appointments, and call your doctor if you are having problems. It's also a good idea to keep a list of the medicines you take. Ask your doctor when you can expect to have your test results.
Where can you learn more?
Go to http://www.healthwise.net/patientEd
Enter A967 in the search box to learn more about "Lung Scan: About This Test".
Current as of: March 26, 2025
Author: Ignite Healthwise, LLC Staff
Clinical Review Board
All Ignite Healthwise, LLC education is reviewed by a team that includes physicians, nurses, advanced practitioners, registered dieticians, and other healthcare professionals.

