Overview
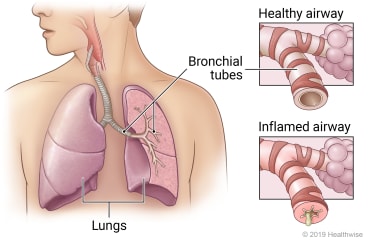
Chronic obstructive pulmonary disease (COPD) is a lung disease that makes it hard to breathe. It is caused by damage to the lungs over many years, usually from smoking.
Sometimes your symptoms may get worse over a short time and stay bad. This is called a COPD exacerbation (say "ig-ZAS-ur-BAY-shun") or flare-up. A flare-up can be dangerous, so it's important to know what to do and take action. Your doctor can help you make a plan to manage flare-ups.
Symptoms of a flare-up include:
- More shortness of breath than usual.
- Coughing more than usual.
- A change in the amount, color, or thickness of mucus.
Many irritants or triggers can cause a flare-up. Common causes are respiratory tract infections such as colds, flu, and pneumonia. Other causes include indoor and outdoor air pollution such as smoke, fumes, and soot.
Follow-up care is a key part of your treatment and safety. Be sure to make and go to all appointments, and call your doctor if you are having problems. It's also a good idea to know your test results and keep a list of the medicines you take.
How can you care for yourself?
- Be safe with medicines. Take your medicines exactly as prescribed. Call your doctor if you think you are having a problem with your medicine. You may be taking medicines such as:
- Bronchodilators. These help open your airways and make breathing easier.
- Corticosteroids. These reduce airway inflammation. They may be given as pills or in an inhaled form.
- Ask your doctor, pharmacist, or respiratory therapist how to use each of your inhalers or nebulizers correctly. With correct use, the medicine is more likely to get to your lungs.
- A spacer may help you get more inhaled medicine to your lungs. Ask your doctor, pharmacist, or respiratory therapist if a spacer is right for you. If it is, ask how to use it properly.
- If your doctor prescribed antibiotics, take them as directed. Do not stop taking them just because you feel better. You need to take the full course of antibiotics.
- If your doctor prescribed oxygen, use the flow rate your doctor has recommended. Do not change it without talking to your doctor first.
- If your doctor has not set you up with a pulmonary rehabilitation program, ask if rehab is right for you. Rehab includes exercise programs, education about your disease and how to manage it, help with diet and other changes, and emotional support.
- If you smoke, try to quit. If you can't quit, cut back as much as you can. Quitting is the most important step you can take to slow the disease and help you feel better. If you need help quitting, talk to your doctor about stop-smoking programs and medicines. These can increase your chances of quitting for good.
- Try to avoid infections such as COVID-19, colds, and the flu. Wash your hands often. You may want to wear a mask when you go to public indoor spaces. Try to avoid sick people.
- Stay up to date on vaccines. This includes getting a flu vaccine every year.
- Try to avoid things that could make your symptoms worse. These include chemical fumes, factory dust, soot, and air pollution. Talk to your doctor about ways to protect yourself if you are exposed to substances that irritate your lungs at home or at work.
- Take care of your teeth and gums. Get regular dental checkups. This can help you stay healthy.
When should you call for help?

Call 911 anytime you think you may need emergency care. For example, call if:
- You have severe trouble breathing.
- You have severe chest pain, or chest pain is quickly getting worse.
Call your doctor now or seek immediate medical care if:
- You have new or worse trouble breathing.
- Your coughing or wheezing gets worse.
- You cough up dark brown or bloody mucus (sputum).
- You have a new or higher fever.
Watch closely for changes in your health, and be sure to contact your doctor if:
- You notice more mucus or a change in the color of your mucus.
- You need to use your antibiotic or steroid pills.
- You do not get better as expected.
Where can you learn more?
Go to http://www.healthwise.net/patientEd
Enter D989 in the search box to learn more about "Chronic Obstructive Pulmonary Disease (COPD) Flare-Ups: Care Instructions".
Current as of: October 25, 2024
Author: Ignite Healthwise, LLC Staff
Clinical Review Board
All Ignite Healthwise, LLC education is reviewed by a team that includes physicians, nurses, advanced practitioners, registered dieticians, and other healthcare professionals.

